- Introduction
- Causes of pancreatic disorder
- Symptoms of pancreatic disorder
- Pancreatic operations
- Why it’s necessary
- Pancreatic Treatment Options
- Candidates for Pancreatic Surgery
- Benefits of Pancreatic Surgery
- Risks of not having surgery
- Risks and Complications
- Post-Operative Care
- Contraindications
- Pancreatic Surgery FAQs
Introduction
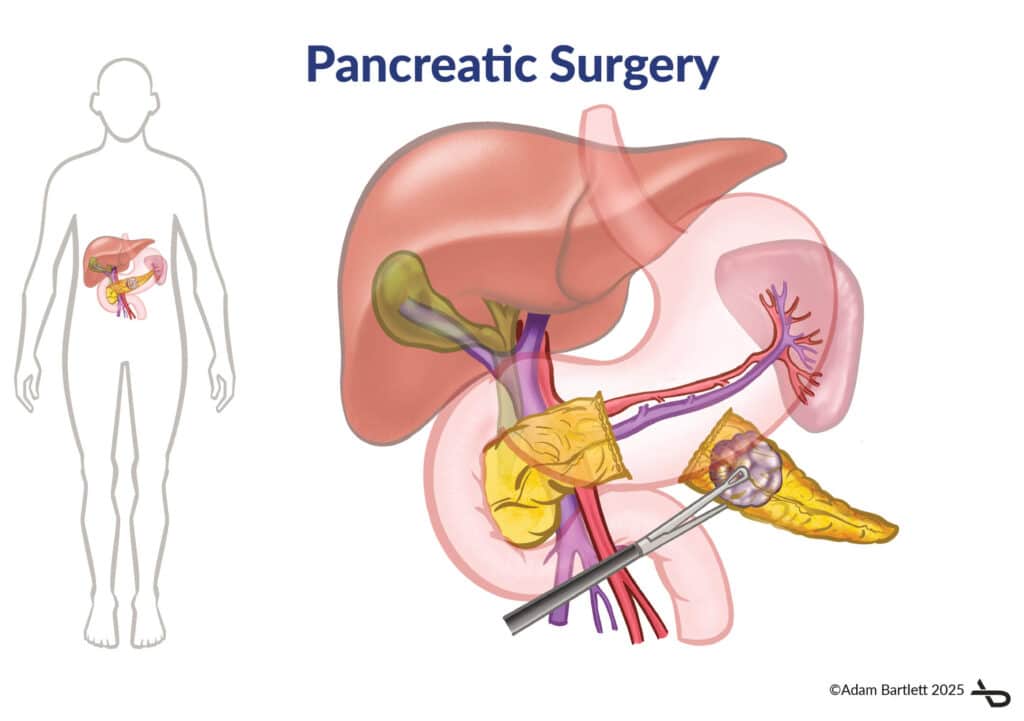
Pancreas is a vital gland, located behind the stomach just below the liver. It produces several digestive enzymes (exocrine function) and also plays a vital role in maintaining the blood glucose levels (endocrine function).
Any disease or injury to the pancreas may cause several problems. Pancreatic surgery comprises a wide range of surgical procedures performed on the pancreas. Most operations involve a resection or removal of the diseased portion of the pancreas. Depending upon the extent of the resection it may have an effect on the exocrine and endocrine function. The exocrine part produces enzymes that help in digestion and absorption of nutrients from food. The endocrine part of the pancreas secretes hormones involved in the metabolism of sugar and maintenance of blood sugar levels.
Make an appointment for your clinical assessment.
Book an appointment
Come in for your assessment
This is where we’ll determine whether you are a suitable candidate for Pancreatic Resection.
Have surgery
Pancreatic surgery is a major operation with significant risks. You will typically be in hospital for 4-6 days.
Come in for a clinical review
Associate Professor Bartlett and your other specialists will continue to be involved in your ongoing care.
Causes of pancreatic disorder
A pancreatic disorder can be caused by either an acute or chronic pathology.
Any inflammation of the pancreas may temporarily block the bile and the pancreatic duct leading to reflux of the bile into the pancreatic duct. Some of the causes of acute injury to the pancreas include excessive consumption of alcohol, certain medications, viral infections such as mumps, also hypothermia and scorpion sting. Alcohol consumption is one of the most common causes of chronic pancreatitis; the other causes of chronic pancreatitis include exposure to industrial toxins, congenital variation in pancreatic duct system and genetic factors. Pancreatic cancer is one of the most common indications of pancreatic surgery.
Symptoms of Pancreatic Disorder
There are no characteristic symptoms attributed to a disorder of the pancreas.
The symptoms are usually generic and may include sharp, aching or burning pain over the upper and central portion of the abdomen associated with back pain. Any enlargement or abnormality of the head of the pancreas may block the bile duct and lead to jaundice associated with dark urine, pale stools and itchy skin. Streatorrhoea is a condition characterized by loose, pale, fatty, floating, offensive bowel motions due to lack of secretion of the digestive juice from the pancreas (exocrine function) that hampers the absorption of fats from the intestines. Pancreatic disorders may interfere with digestion and sugar metabolism and the patient experiences weight loss and loss of appetite.
Pancreatic Operations
Some of the commonly performed pancreatic operations include pancreatico-dudenectomy (Whipple’s procedure), distal pancreatectomy, pancreatic bypass, pancreatic necrosectomy, and drainage of pseudocysts.
Depending upon the indication for surgery, the type of operation will differ. A/Professor Adam Bartlett will explain this at the time of your consultation.
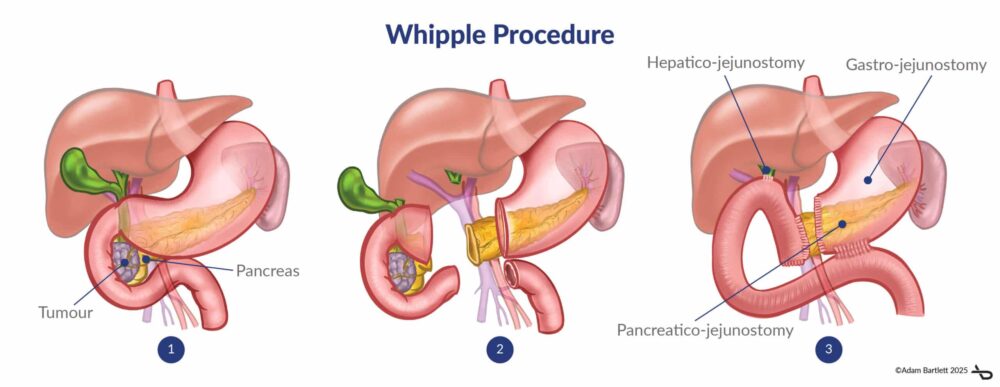
Whipples Procedure (Pancreaticoduodenectomy)
Pancreatico-dudenectomy, more commonly referred to as Whipple’s procedure, is the most common pancreatic surgery indicated for the removal of tumors from the head of the pancreas. Distal pancreatectomy involves resection of the tail and body of the pancreas, leaving the head. Pancreatic bypass is a palliative operation, that is rarely performed, to bypass an obstructing tumour located within the head of the pancreas. Pancreatic necrosectomy is usually performed in an acutely unwell patient with severe acute pancreatitis. Drainage of pseudocysts is a surgical procedure performed in patients with a collection of inflammatory fluid around the pancreas as a consequence of acute pancreatitis. It is usually performed endoscopically using EUS.
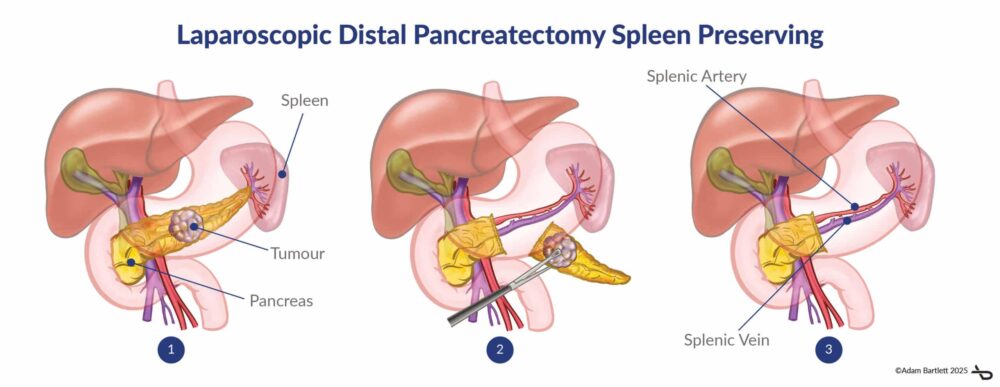
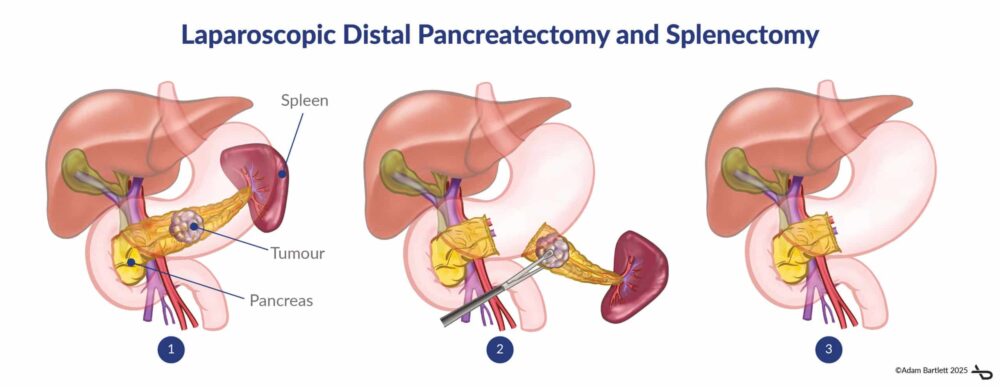
Distal Pancreatectomy
This involves resection of the tail and body of the pancreas, leaving the head intact. It is often used for tumours or cysts in the tail of the pancreas and may include removal of the spleen if involved. The procedure can often be performed laparoscopically or robotically, reducing recovery time. When the tumour is more advanced it may require an open operation.
Pancreatic Bypass
A palliative operation, rarely performed, to bypass an obstructing tumour in the head of the pancreas. This may involve creating a connection between the stomach and small intestine (gastrojejunostomy) or between the bile duct and small intestine (choledochojejunostomy) to relieve symptoms of or obstruction or jaundice, respectively.
Pancreatic Necrosectomy
Performed in acutely unwell patients with severe acute pancreatitis. This procedure removes necrotic (dead) pancreatic tissue to prevent infection and sepsis. It is often done in stages and may require intensive care support.
Drainage of Pseudocysts
A surgical procedure for patients with inflammatory fluid collections around the pancreas, often performed endoscopically using endoscopic ultrasound (EUS), as a consequence of acute pancreatitis. It involves placing a stent or drain to allow the cyst to empty into the stomach or duodenum.
Why is Pancreatic Surgery Necessary?
Pancreatic surgery is necessary to treat conditions that cannot be managed with medication or less invasive methods alone. Common indications include pancreatic cancer (such as adenocarcinoma), chronic pancreatitis causing severe pain or complications, acute pancreatitis with necrosis, pancreatic cysts or pseudocysts at risk of rupture or infection, and benign tumours like intraductal papillary mucinous neoplasms (IPMN). Without surgery, these conditions can lead to life-threatening complications such as obstruction, infection, or metastatic spread. The goal is to remove diseased tissue while preserving as much pancreatic function as possible.
Pancreatic Treatment Options
Treatment for pancreatic disorders depends on the underlying cause, severity, and patient’s overall health. Options include non-surgical and surgical approaches.
Non-Surgical Pancreatic Treatment
Non-surgical options may be used for symptom management or in patients unsuitable for surgery. These include:
- Pain relief with analgesics or nerve blocks.
- Enzyme replacement therapy for exocrine insufficiency (Creon).
- Insulin therapy for endocrine dysfunction leading to diabetes.
- Endoscopic procedures, such as ERCP (endoscopic retrograde cholangiopancreatography) for stent placement to relieve duct obstruction.
- Chemotherapy or radiation therapy for inoperable pancreatic cancer.
- Lifestyle modifications, including alcohol cessation and dietary changes.
Surgical Pancreatic Treatment
Surgical treatment is often curative or palliative and includes the procedures outlined in the Pancreatic Operations section. Laparoscopic or robotic-assisted techniques may be used for less invasive resections, reducing recovery time and complications. Major resections like the Whipple’s procedure are performed open for complex cases.
Is Everyone a Candidate for Pancreatic Surgery?
Not everyone is a candidate for pancreatic surgery. Suitability depends on factors such as the stage and location of the disease, overall health, liver and kidney function, nutritional status, and presence of comorbidities like cardiovascular disease or obesity. Patients with advanced metastatic cancer, severe chronic liver disease, or poor performance status may not benefit from surgery due to high risks. A thorough preoperative assessment, including imaging (CT, MRI, PET scans), blood tests, and sometimes a biopsy, is essential. Associate Professor Adam Bartlett will determine candidacy during consultation.
Benefits of Pancreatic Surgery
Pancreatic surgery offers several benefits, particularly for resectable diseases:
- Potential cure for localised pancreatic cancer, with 5-year survival rates improving to 20–30% post-resection compared to less than 5% without surgery.
- Relief from symptoms such as pain, jaundice, and digestive issues.
- Prevention of complications like infection or obstruction.
- Preservation of quality of life by removing diseased tissue and restoring normal function where possible.
- In cases of chronic pancreatitis, reduced need for long-term pain management and improved nutrition.
Risks of Not Having Pancreatic Surgery
Delaying or avoiding pancreatic surgery when indicated can lead to disease progression, including:
- Spread of cancer (metastasis) to other organs, reducing survival chances.
- Worsening pain, weight loss, and malnutrition from impaired digestion.
- Complications such as bowel obstruction, jaundice, or ascites.
- Life-threatening events like pancreatic necrosis, infection, or haemorrhage in acute cases.
- Development of diabetes or exocrine insufficiency, impacting long-term health.
Risks and Complications of Pancreatic Surgery
All surgeries carry risks, and pancreatic procedures are complex with a higher complication rate (up to 30–50%) due to the organ’s location and functions. Risks are minimised through having your procedure done with experienced surgical teams, such as Associate Professor Adam Bartlett.
General Risks of Surgery
These include:
- Wound infection.
- Deep vein thrombosis (DVT) or pulmonary embolism.
- Anaesthetic complications, such as allergic reactions or respiratory issues.
- Development of a hernia at the incision site.
- Increased risks if overweight, smoking, or with comorbidities.
Specific Risks and Complications from Pancreatic Surgery
Specific complications may occur in 20–40% of cases and include:
Bleeding
Intraoperative or postoperative haemorrhage, occurring in 5–10% of cases, due to the pancreas’s vascular nature. This may require blood transfusion or reoperation.
Infection
Postoperative infections, such as abscesses or peritonitis, in 10–15% of patients. Managed with antibiotics or drainage.
Pancreatic Leakage
Also known as pancreatic fistula, where digestive enzymes leak from the resection site (10–20% incidence). This can cause abdominal pain, fever, and delayed healing, often requiring drains or further intervention.
Delayed Gastric Emptying
Affecting up to 20% of Whipple’s procedure patients, where the stomach takes longer to empty, leading to nausea and vomiting. Usually resolves with time and nutritional support.
Diabetes or Digestive Issues
New-onset diabetes (10–20%) or exocrine insufficiency (steatorrhoea) due to removal of pancreatic tissue, requiring insulin or enzyme supplements.
Respiratory Complications
Pneumonia or atelectasis in 5–10% of cases, particularly after major resections. Early mobilisation and physiotherapy help prevent this.
Post-Operative Care
After pancreatic surgery, patients are monitored in a high-dependency unit or intensive care for 1–2 days. Key aspects include:
- Pain management with epidural analgesia or patient-controlled analgesia (PCA).
- Intravenous fluids and gradual reintroduction of oral intake, often starting with clear fluids.
- Monitoring for complications via blood tests, drains, and imaging.
- Early mobilisation to prevent DVT and respiratory issues.
- Nutritional support, possibly via nasogastric tube or total parenteral nutrition (TPN).
- Hospital stay typically 7–14 days; follow-up includes wound checks and dietary advice. Avoid heavy lifting for 6 weeks and resume driving when comfortable.
Contraindications for Pancreatic Surgery
Pancreatic surgery may be contraindicated in:
- Advanced metastatic disease where resection is not curative.
- Severe comorbidities, such as uncontrolled heart failure, renal failure, or advanced cirrhosis.
- Poor nutritional status or cachexia increasing operative risks.
- Patient refusal or inability to tolerate anaesthesia.
- Inoperable tumours encasing major vessels like the superior mesenteric artery.
Pancreatic Surgery FAQs
What is the Goal of Performing Pancreatic Surgery?
The primary goal is to remove diseased tissue (e.g., tumours or necrotic areas) to achieve cure, relieve symptoms, or prevent complications, while preserving pancreatic function.
How is the Pancreas Divided Up?
The pancreas is anatomically divided into the head (near the duodenum), uncinate process, neck, body, and tail (near the spleen). Surgery targets specific sections based on disease location.
What Patients Require Pancreatic Surgery?
Patients with resectable pancreatic cancer, chronic pancreatitis unresponsive to medical therapy, acute necrotising pancreatitis, or symptomatic cysts/pseudocysts typically require surgery.
How Long is the Hospital Stay After Pancreatic Surgery?
Hospital stay varies: 4–7 days for minor procedures like distal pancreatectomy, and 10–14 days or more for major resections like Whipple’s, depending on complications.
What Preparations are Needed Before Surgery?
Preparations include preoperative imaging, blood tests, nutritional optimisation, smoking cessation, and sometimes neoadjuvant chemotherapy. These will all be outlined by A/Professor Adam Bartlett
How is Pain Managed After Surgery?
Pain is managed with epidural anaesthesia, intravenous opioids via PCA, and oral analgesics as recovery progresses. Multimodal approaches reduce opioid use.
When Can I Resume Normal Activities?
Light activities can resume within 2–4 weeks; full recovery takes 6–12 weeks. Avoid strenuous exercise or heavy lifting until cleared by your surgeon.
Will I Need Chemotherapy or Other Treatments?
For pancreatic cancer, adjuvant chemotherapy is often recommended post-surgery to improve outcomes. Radiation may be used in select cases.
When Should I Seek Medical Help After Surgery?
Seek immediate help for severe pain, fever >38°C, wound redness/discharge, persistent vomiting, jaundice, shortness of breath, or leg swelling. Contact the clinic or emergency services.
Make an appointment for your clinical assessment.
Book an appointment
Come in for your assessment
This is where we’ll determine whether you are a suitable candidate for Pancreatic Resection.
Have surgery
Pancreatic surgery is a major operation with significant risks. You will typically be in hospital for 4-6 days.
Come in for a clinical review
Associate Professor Bartlett and your other specialists will continue to be involved in your ongoing care.